Does Laser Lipo Work? -in Forbes Health
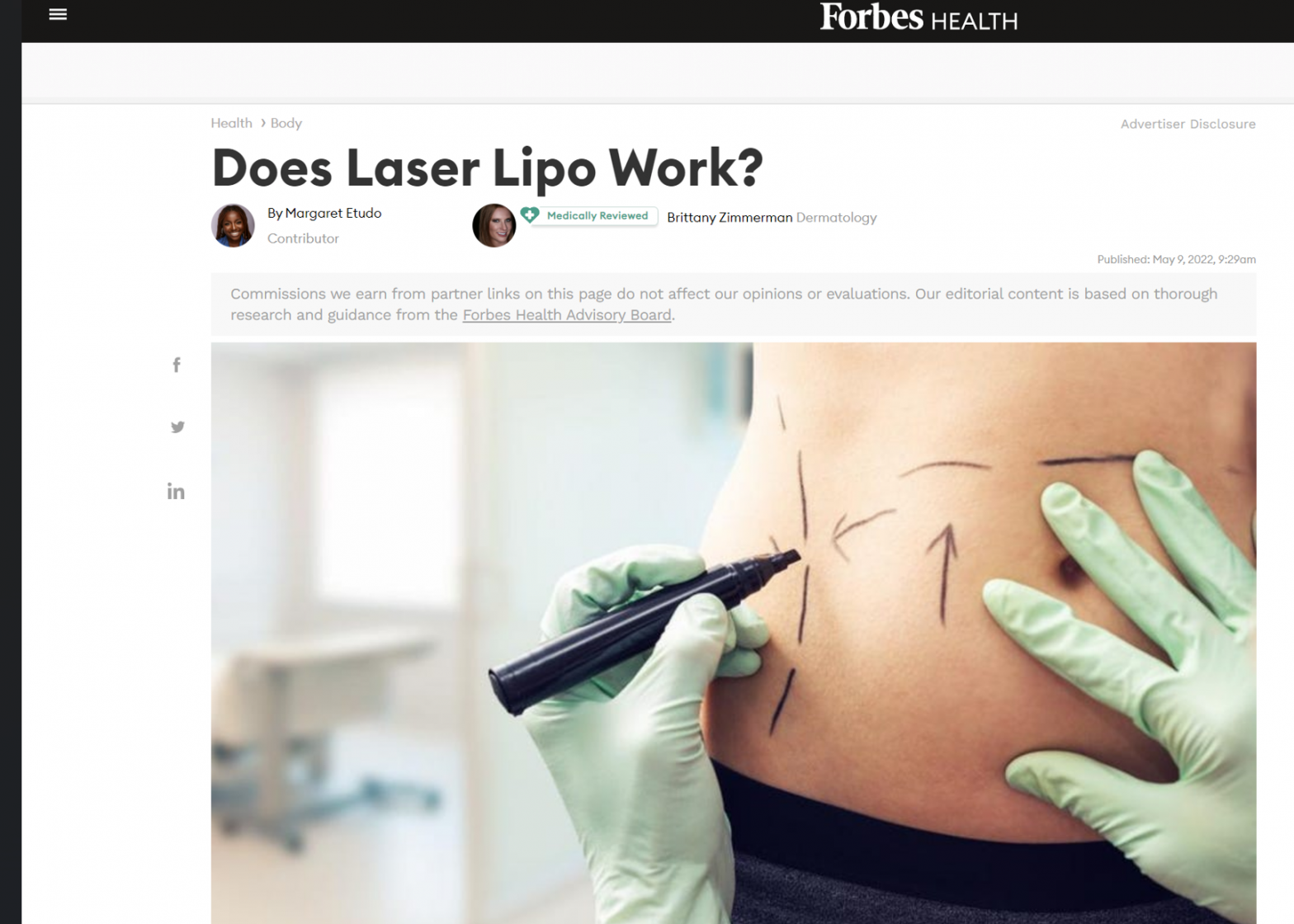
09 May 2022 By Margaret Etudo in Forbes Health about Smartlipo by Mr Ayham Al-Ayoubi. Laser liposuction, also referred to as laser lipo, is a fat reduction technique and less traumatic, less invasive option than traditional liposuction. The procedure is also noted to lead to less swelling and bruising and require less recovery time than… Read more… Does Laser Lipo Work? -in Forbes Health
Categorized as Media Articles
Kim Kardashian is the world’s most recognisable woman
Her exceptional figure has always been a…
Categorized as Media Articles
‘Covid Face’ – How we aged six years in six months
Dr Ayoubi about Covid Face – October 2020
Categorized as Media Articles
SmartSkin C02 Fractional Laser with No Downtime, No Redness and No Peeling
Dr Ayoubi about C02 Laser – July 2018
Categorized as Media Articles
The Future of Non-Surgical Face Lift
Dr Ayoubi explains Silhouette Soft – January 2018
Categorized as Media Articles
Fast-Track To Bikini-Ready
Dr Ayoubi about Cellulaze laser- December 2017
Categorized as Media Articles
Saving Face by Sculptra
Dr Ayoubi in The Times on Sculptra – November 2017
Categorized as Media Articles